
A subject’s arm is shown positioned on the platform of the Berkeley Lab instrument. Artificial pulses are applied by the actuator and detected by an ultrasound probe.
APPLICATIONS OF TECHNOLOGY:
- Detects cardiovascular disease (CVD) at the preclinical stage by measuring vasorelaxation
- Monitors the effects of statins and other drugs, vitamins, exercise, and the cessation of smoking on arterial function
- Compares pulse transit times in the limbs of a patient to detect occlusion
ADVANTAGES:
- Only noninvasive vasorelaxation assessment technique to equal or exceed the accuracy of invasive methods
- Can be manufactured for under $5,000, approximately one-fifteenth the cost of ultrasound imagers
- 37% greater sensitivity to endothelium-mediated vasorelaxation than the brachial artery (BA) imaging method
- Does not require experienced operators or an ultrasound technician
ABSTRACT:
Jonathan Maltz and Thomas Budinger of Berkeley Lab have invented the only noninvasive vasorelaxation assessment technique to achieve the previously unprecedented accuracy of invasive methods that use artificial pulses to obtain pulse wave velocity. The Berkeley Lab method will enable the inexpensive and routine detection and monitoring of preclinical cardiovascular disease (CVD) via endothelial function. It can also be used to assess the efficacy of statins and other regimens for aiding arterial health as well as for detecting occlusion in limbs.
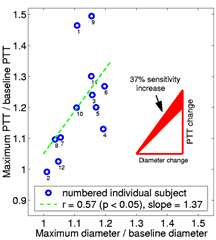
Comparing the sensitivity of artificial PTT with artery diameter measurements
Berkeley Lab studies on human subjects have verified that the new method is 37% more sensitive to arterial relaxation than brachial artery (BA) imaging. In addition, the apparatus costs one fifteenth as much as an ultrasonic imager, minimizes the possibility of human operating error, and eliminates the need for an ultrasound technician.
The Berkeley Lab method works by inducing an artificial pulse at the superficial radial artery via a linear actuator. A natural pulse is not used because it changes the properties of the artery wall and its edge is not as sharp and easy to measure. An ultrasonic Doppler stethoscope detects the pulse 10-20 cm upstream from the initial pulse. The delay between pulse application and detection provides the pulse transit time (PTT). PTT is measured before and after five minutes of BA occlusion and reactive hyperemia. The Berkeley Lab instrumentation includes a cuff occlusion system but other means of stimulating endothelial mediated compliance changes are possible.
As the blood flow increases after occlusion, the endothelial cells that line the inner wall of the artery sense the increased friction and chemical composition of the blood and release relaxing agents into the artery’s smooth muscle. The healthier the arterial system, the better the endothelial layer functions and the greater the difference will be between the pre-and post-occlusion measurements.
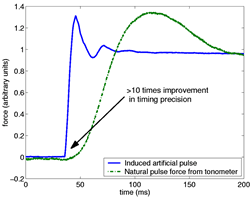
Timing precision of artificial and natural pulses
The rise time of the artificial pulse used in the Berkeley Lab method is more than an order of magnitude shorter than that of a natural pulse. The ability to calculate PTT from artificial pulses makes the Berkeley Lab technique much more precise than other noninvasive procedures.
At present, the most common method of assessing endothelium-mediated vasorelaxation is BA imaging, which involves taking high resolution ultrasound images to determine the diameter of the brachial artery before and after several minutes of arterial occlusion. However, statistical analysis of the measurements using the ultrasound technique indicate that this method is too sensitive to differences in methodology to allow its routine use in a clinical setting.
In contrast, tests with a Berkeley Lab prototype show only a 3% variation in same-day results when operators remain the same or when they are changed. When the same subjects are tested on different days, a 4% variation is observed. Operators with less than 30 minutes of training were employed in the studies. The Berkeley Lab technique also has the advantage of a timing precision of approximately 1 ms compared to 10 ms for natural-pulse based methods.
Impairment of arterial endothelial function is an early event in atherosclerosis and correlates with the major risk factors for CVD. It is also one of the earliest predictors of CVD and coronary events. In addition, factors that are considered beneficial to cardiovascular health, such as exercise, appear to improve endothelial function.
A device based on this technology was further developed by a former licensee. The following are available to new licensees:
- Prototypes
- Data on prototype performance
- Clinical trial data and documents indicating patient response and equivalence to ultrasound method
- Communication with the FDA regarding approval of the device for clinical trial
- Engineering drawings, including editable CAD files for chassis, electronic schematics
- Source code, application source, and firmware source
STATUS:
- Issued U. S. Patent 8,666,472.
- Licensed in the field of human medical diagnostics and vascular health monitoring.
FOR MORE INFORMATION:
REFERENCE NUMBER: IB- 1796
RELATED TECHNOLOGIES:
Assessing Endothelial Function with a Standard Blood Pressure Cuff, IB-2772
Software Suite for Endothelial Function Assessment 2015-162
